|
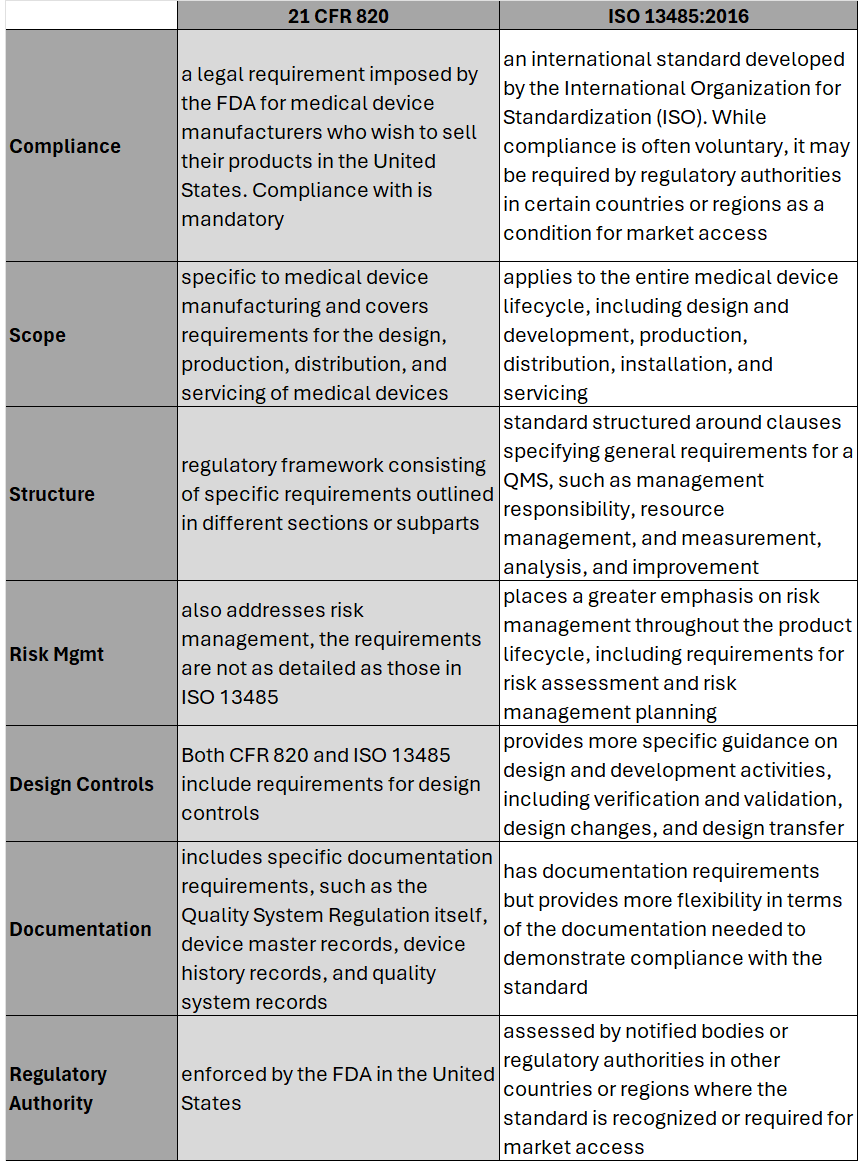
On February 2nd, 2024 the U.S. Food and Drug Administration (FDA) made its formal announcement and ruling providing guidance on 21 CFR Part 820 which up to that point was the standard overseeing medical device quality system regulation and current good manufacturing practices (cGMP) in the United States of America. The big news – 21 CFR 820 will be heavily amended to incorporate ISO 13485 as the leading guidance for Quality Management System Regulation (QMSR) and cGMP. While the news wasn’t a surprise, it does put a final note on the direction the agency intends to take for medical device practices moving forward, especially as it relates to risk management. While many device OEMs already utilize ISO as their leading regulation standard, those who don’t will have two years to adjust to these changes to be in compliance effective February 2nd, 2026. Here’s what you need to know as it relates to the differences between 21 CFR 820 and ISO 13485, as well as considerations OEMs should take into account in order to meet the 2026 deadline. Big Picture:
Key Differences: Transitioning to ISO 13485 Transitioning from CFR 820 to ISO 13485 involves several steps to ensure compliance with the ISO standard. A general outline of the steps an OEM should take to transition may include: 1. Understand the Requirements of ISO 13485: Familiarize yourself with the requirements of ISO 13485. This includes understanding the structure of the standard, its key clauses, and any specific requirements which may differ from CFR 820. (see above table for highlights) 2. Gap Analysis: Conduct a thorough gap analysis to identify the differences between your current quality management system under CFR 820 and the requirements of ISO 13485. This will help you determine what changes, if any, need to be made to your existing processes, procedures, and documentation. This is also a great time to do a review of your QMS tool to determine if it is an appropriate tool for future use. 3. Document Review and Update: Review your existing documentation, including quality manuals, procedures, work instructions, and forms, to ensure they align with the requirements of ISO 13485. Update or create new documents as necessary to meet the standard's requirements. 4. Training and Awareness: Provide training to relevant personnel to ensure they understand the requirements of ISO 13485 and their roles in implementing and maintaining the QMS. This may include training on new procedures, processes, and documentation. 5. Implementation of New Processes: Implement any new processes or procedures required by ISO 13485. This may include processes related to risk management, design and development, purchasing, production, and service provisions. 6. Internal Audits: Conduct internal audits of your QMS to verify compliance with ISO 13485 requirements. Identify any non-conformities and take corrective actions to address them. 7. Management Review: Hold management reviews to evaluate the effectiveness of the QMS and identify opportunities for improvement. Ensure top management is actively involved in the transition process and committed to maintaining the QMS. 8. Certification Audit: BEFORE you consider this step be sure to speak with a regulatory affairs subject matter expert to ensure it is necessary. Once you believe your QMS is fully compliant with ISO 13485, engage a certification body to conduct a certification audit. The audit will assess your organization's compliance with the standard and determine if you are eligible for certification. 9. Address Non-conformities: If any non-conformities are identified during the certification audit, take corrective actions to address them. The certification body will typically require verification that corrective actions have been implemented before issuing the ISO 13485 certificate. 10. Continual Improvement: Continuously monitor and improve your QMS to ensure ongoing compliance with ISO 13485 and to enhance the efficiency and effectiveness of your processes. Although the 21 CFR 820 and ISO 13485 vary in their structure, and at times use different terminology to describe similar concepts, 21 CFR 820 and ISO 13485 are substantially similar in that both prioritize principles such as risk management, design controls, and continual process improvement. It’s possible as organizations begin to look at their current standards and systems, they will find the transition process is not as cumbersome as initially thought. While this is an obvious assumption, it’s important to note regulatory affairs professionals should be counseled throughout this entire process to ensure appropriateness of adoption and change management.
0 Comments
Here’s a challenge I see quite often while we’re on a client project involving mechanical design or CAD work. Does this familiar? Someone is tasked with designing a new sub-assembly or component for an existing product. As they get underway their work on face value gets the company to a conclusion where the design/ drawing is technically complete. As such, this person is able to check the proverbial box for ‘task completed’ and move on to the next assignment. While the work may have technically been completed, it often is done in a fashion which causes all sorts of problems down the road for the company, including other employees working on the same project within the same organization as well as their external suppliers. How is it someone can complete a design project satisfactory on the surface yet problems arise down the road with that very same design, which had been previously approved? Answer: the devil is in the details, or lack thereof, to be more specific. The reason why companies and or their respective employees experience this is because they aren’t following a formal and documented ‘gold standard’ for their product design practices. Simply put, they lack discipline with design fundamentals. As a result of a lack of design standards (and perhaps training) employees are left to decide for themselves how to complete a task which may get them to the finish line but the approach, process and details along the way can have wild variances and interpretations. While this may be commonplace and old news to many of you reading this article, the reality is the actual practice of designing a product with repeatable ‘gold standards’ is anything but common sense or consistent in the workplace. When our approach to design is fast and loose we experience the following:
When these issues show up it causes companies to reinvest dollars and resources into their work in order to move the project forward to get it to a point of where it can be properly advanced along the product development life cycle. This reinvestment is unnecessary and a huge time suck. We see this a lot when a medical device OEM has a contract manufacturer (CM) do some of their design work. In more times than I can count the work which is produced in this scenario is rough, limited with detail and documentation, almost never parametrically driven, and close to useless in other scenarios. Don’t fall for the trap of “we just need drawings.” While that may be the case in the moment, this will almost always cause you more work and funds down the road. For these reasons it’s vital companies implement a ‘gold standard’ in their design work which their employees and suppliers follow to ensure the work each party is facilitating makes it to the finish line in the same format, intent and approach. This unification of process increases the likelihood design work is done correctly while also ensuring future usage of said designs doesn’t require additional unnecessary iterations or complete redesigns. If implementing a ‘gold standard’ for your design and product development practices could be a benefit to your team or company, here are some of the key points to consider:
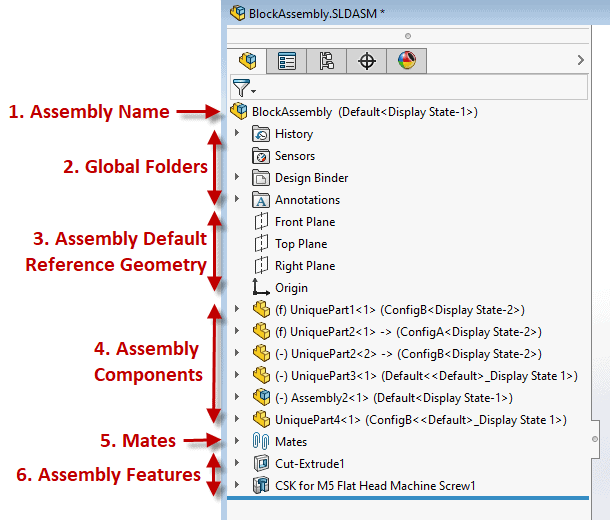
Example below: A well laid out Solidworks Assembly Feature Manager Design Tree If you, and or your company, lacks a ‘gold standard’ for your product design efforts you are inevitably wasting time and resources. This also has a direct correlation to a suppliers’ ability to help with outsourced work causing the overall project to be more challenging and lengthier than necessary (prototyping, manufacturing, etc.) While this isn’t a fun realization there is hope! Here’s how to fix it. Start right away by developing a best practice plan. This will help you and your team form an outline for what design practices and approaches are ideal for your product and technology, which aren’t, etc. From there setup a review plan to provide feedback on all work performed. Once the infrastructure of your new gold standard system is established you’ll want to asses the skills of your team and develop a training program which can be offered to both new and existing employees. Medtech Snapshot: Fundraising and the Sales Funnel with Scott Nelson, CEO Fastwave Medical1/15/2024 Medtech Snapshot episode #22 features Fastwave Medical's CEO Scott Nelson sharing insights on the impact of using the 'sales funnel' process for medical device fundraising purposes. Listen how Scott's approach to fundraising starts off by casting a wide net via branding and mission/ story telling efforts then intentionally narrows the funding field to a smaller audience of potential investors which are aligned with his company's mission. Want more info? Check out Square-1's other Medtech Snapshot episodes at https://www.sqr1services.com/white-papers/category/snapshot Learn about Fastwave Medical's mission and product offering at https://www.fastwavemedical.com/ The quickest way to overcome a business challenge is to get help from those who are experienced in besting your beast! The team at Square-1 Engineering is comprised of a variety of technical and project management professionals who are subject matter experts in the areas of NPD, Quality, Compliance and Manufacturing Engineering.
Learn more about how we can solve your work and project problems today to get you back on track! VISIT HERE Ensuring the smooth progression of a medical device through product development is more than just having a good idea and the money to back it up. In the ever-evolving landscape of healthcare, the development of cutting-edge medical devices demands a strategic and disciplined approach. At the heart of this process lies several key drivers each with their own distinctive value, yet all of which work in harmony bringing us to the conclusion we are hoping for - getting our products successfully through each phase of product development and eventually out the door to patients in need. This article explores the 'key drivers' which will keep your product development efforts successfully moving forward. Let’s begin with looking at what may very well be an obvious statement – what problem are you trying to solve and is it worth solving in the first place. The second portion of this question is key – is the problem you want to solve, via the technology you intend to develop, actually worth solving. Some advice – not all problems are worth solving, especially in the eyes of investors. It’s going to take deep pockets to build a product, upwards of $100 million on average for a PMA device, which is why its so important to be able to confidently answer this first two-part question: what problem are you trying to solve and is it worth solving in the first place. Once you know your technology front and back, understand the macroeconomics associated with it, it’s time to put a well-crafted plan into place to help keep you on track throughout each phase of the development cycle. Here enters project management. Project management plays a critical role in the success of medical device product development as it holds your team accountable to keeping focused on the key strategies which contribute to a seamless progression from concept to market. This should include: Developing A Clear Project Plan A well-defined roadmap is the cornerstone of any successful project as it delineates tasks, milestones, and dependencies. Roles and responsibilities are outlined, laying the groundwork for a collaborative and efficient work environment. Regular updates and adjustments ensure the plan can accommodate change while staying aligned with the overarching project goals. Timely Decision-Making Delays are costly endeavors. Projects which embrace prompt decision-making empower team members to make informed choices within their spheres of expertise. This can minimize bottlenecks, fostering an environment where decisions were made swiftly, keeping the project on a forward trajectory. Risk Management A robust risk management plan provides continuous assessment of potential challenges. Glen Rabito, COO of Nidus Biomedical, advises “identify the top three (3) risks and go tackle those things first. This will allow us to understand the technical and clinical risks” [associated with the development of your technology]. Effective Communication Clear and transparent communication is the lifeblood of successful projects. Regular team meetings facilitate discussions on progress, challenges, and potential solutions, creating an environment where everyone is well-informed and engaged. Resource Allocation Efficient resource allocation is essential for maintaining momentum throughout the development process. Teams which carefully monitor the allocation of human, financial, and technological resources tend to fare better than those who don’t. Also, what should you keep internally as a core competency versus outsource to someone better set up to facilitate a portion of your work. Adaptability Flexibility in the face of change is a hallmark of successful product development efforts. Project plans should be designed to be adaptable allowing the team to accommodate shifts in scope, requirements, or unforeseen economic challenges. Regulatory Compliance Navigating the complex landscape of medical device development requires a keen understanding of regulatory requirements. Staying informed of regulations and incorporating specific milestones related to regulatory submissions in the project plan is crucial to your success in keeping things moving forward. Prototyping and Iterative Development Teams which embrace an iterative development approach are focused on continuous improvement, allowing the team to make necessary adjustments based on user and stakeholder input. The result is a product which meets regulatory standards AND user needs and expectations. Quality Assurance and Testing Ensuring the highest quality standards is non-negotiable. Thorough quality assurance and testing processes should be integrated at every stage, whereas multiple testing iterations are planned for and issues identified during testing are promptly addressed. Documentation and Traceability Many of us love to gloss over this step – yet doing so is a monstrous mistake. A disciplined approach to documentation is critical for accountability and traceability. A team which maintains accurate and up-to-date documentation throughout the project, establishing clear traceability between milestones, design inputs, and verification/validation activities will be better positioned for success down the road, while mitigating project efforts being put on hold. In the intricate dance of medical device development and effective project management is the guiding force which better positions your team and company for success. The strategies outlined above, from meticulous planning to continuous improvement, collectively contribute to the seamless progression of a product and the overarching project. As the healthcare landscape continues to evolve, these principles will remain essential for navigating the complexities of medical device development and delivering innovations which make a lasting impact on patient care. The quickest way to overcome a business challenge is to get help from those who are experienced in besting your beast! The team at Square-1 Engineering is comprised of a variety of technical and project management professionals who are subject matter experts in the areas of NPD, Quality, Compliance and Manufacturing Engineering. Learn more about how we can solve your work and project problems today to get you back on track!
Medtech Snapshot: Forward Progress in Product Development with Glen Rabito, COO of Nidus Biomedical1/10/2024 Medtech Snapshot episode #21 features Nidus Biomedical COO Glen Rabito talking through the five considerations to keep product development moving forward, especially in the early phases of development.
#medtech #snapshot #medicaldevice #productdevelopment #NPD #riskmanagement #userneeds #patientsafety Episode #20 of Medtech Snapshot features Peman Montazemi, CTO of Bright Uro - overcoming some of the biggest software development challenges for medical device applications.
#software #embeddedsystem #medicaldevice #snapshot #medtechsnapshot #medtech #softwaredevelopment #engineering #newproductdevelopment #regulation #cybersecurity #samd #spdf Episode 19 of Medtech Snapshot features Scott Nelson, CEO of FastWave Medical sharing insights on the strategy of operating in stealth mode versus public for a medical device start-up.
Are you liking these Medtech Snapshot digests? Check out our archives for more 3 minutes snip-its at https://lnkd.in/gFwF9GYN #snapshot #medtech #medtechsnapshot #startup #stealth #strategy #medicaldevice The art of attracting talent! Nuvaira, Inc. CEO Dennis Wahr M.D. joins us on Medtech Snapshot to discuss strategies in attracting great talent into a small company, especially how to lure talent away from big businesses. Check out https://lnkd.in/gFwF9GYN for our past episodes of Medtech Snapshot. #medtech #news #strategy #talent #hiring #snapshot #podcast The quickest way to overcome a business challenge is to get help from those who are experienced in besting your beast! The team at Square-1 Engineering is comprised of a variety of technical and project management professionals who are subject matter experts in the areas of NPD, Quality, Compliance and Manufacturing Engineering. Learn more about how we can solve your work and project problems today to get you back on track! VISIT HERE Medical device companies play a critical role in advancing healthcare as their ability to diagnose, monitor, and treat medical conditions allow patients like you and I the opportunity to recover and live longer. Device companies carry a heavy burden on our behalf and that burden starts with product risk. One of the biggest challenges an OEM medical device organization will be faced with is managing risk, especially during the early stages of product development. The integration of risk management into design control (ISO 14971) is essential for identifying, assessing, and mitigating potential risks associated with the design and development of a medical device. Given risk management is a part of nearly every development process, and is a primary focus of all regulatory agencies like the U.S. Food and Drug Administration (FDA) and the European Medicines Agency (EMA), why is it then so many medical device companies struggle with sound risk management strategies? The failure to address risks adequately can lead to a whole host of problems ranging from regulatory non-compliance, compromised patient safety, financial setbacks, and in severe situations criminal prosecution of executives. Needless to say, understanding why medical device companies come up short with their risk management strategy and how you can avoid that for yourself is key to your future success. In this article, we will explore some of the key reasons behind risk management failure. Most Common Risk Failure Factor - Inadequate Understanding of Regulatory Requirements: One of the primary reasons for failure in risk management is an insufficient understanding of the complex and evolving regulatory landscape. Medical device companies must navigate a web of regulations, standards, and guidelines to ensure compliance. Failing to keep abreast of these requirements can result in flawed risk assessments, inadequate risk mitigation measures, and ultimately, regulatory sanctions. Poor Integration of Risk Management into Product Development: Successful risk management should be an integral part of the product development lifecycle. However, some companies make the mistake of treating it as a standalone process rather than integrating it seamlessly into every stage of development. When risk management is an afterthought, essential risks may be overlooked, leading to suboptimal product designs, increased failure rates, and compromised patient outcomes. Lack of Cross-Functional Collaboration: Effective risk management requires collaboration across various departments, including research and development, regulatory affairs, quality assurance, and manufacturing. Failure to establish clear communication channels and encourage cross-functional collaboration can result in siloed decision-making. This lack of coordination can lead to critical risks being underestimated or missed entirely. Insufficient Resources and Expertise: Some medical device companies fail in risk management due to resource constraints and a shortage of expertise. This can manifest in inadequate training for personnel responsible for risk management, insufficient allocation of time and budget, and a lack of access to external expertise. Without the necessary resources, companies may struggle to conduct comprehensive risk assessments and implement effective risk mitigation strategies. Overemphasis on Short-Term Goals: Pressure to meet short-term financial goals can sometimes lead companies to prioritize speed to market over thorough risk analysis. This can result in hasty decision-making and inadequate risk identification and mitigation. Companies need to strike a balance between meeting market demands and ensuring the safety and efficacy of their medical devices in the long run. Failure to Learn from Industry Incidents: The medical device industry has witnessed several high-profile incidents related to product failures and patient harm. Failure to learn from these incidents and implement lessons learned into future risk management strategies can perpetuate the same mistakes. Companies must actively analyze industry incidents, update risk management processes accordingly, and continuously improve their practices. Ineffective Communication with Stakeholders: Communication is crucial in risk management, both internally and externally. Companies that fail to communicate effectively with their stakeholders, including regulatory bodies, healthcare professionals, and patients, may face increased scrutiny and regulatory challenges. Transparency and open communication are essential for building trust and demonstrating commitment to patient safety. In the highly regulated and dynamic field of medical devices, effective risk management is not just a regulatory requirement - it is a fundamental aspect of ensuring patient safety and the success of a company. Understanding the pitfalls that lead to failures in risk management can help medical device companies proactively address these challenges. By prioritizing compliance, integrating risk management into every stage of product development, fostering cross-functional collaboration, and learning from industry incidents, companies can enhance their risk management strategies and contribute to the advancement of healthcare with safe and reliable medical devices. The quickest way to overcome a business challenge is to get help from those who are experienced in besting your beast! The team at Square-1 Engineering is comprised of a variety of technical and project management professionals who are subject matter experts in the areas of NPD, Quality, Compliance and Manufacturing Engineering. Learn more about how we can solve your work and project problems today to get you back on track!
Executive Summary
Developing a strategic and consistent process to evaluate and therefore acquire suppliers before you need them is vital to our ability in growing our respective companies. When we utilize a systematic process we eliminate bias and emotion from the decision making process which allows us to make decisions which are capabilities and needs based rather than emotions. Your ‘minimum expectations’ list serves as a road map for decision making and comparison shopping as you engage with each supplier. Developing A Supplier Selection Process The supplier selection process is an important and vital step for any size company. Making the wrong decision leads to countless hours of wasted time and of course money down the drain. A successful supplier selection process is even more important for small and startup based business where financial considerations are at the top of the pecking order. When looking for a new supplier follow these steps to best position yourself and company for success: Know What You Need Before You Need It Two reasons this is important: 1st – if you don’t know what you need how will you be able to explain it to a supplier? When we know what we need and want we are better prepared to explain those needs accordingly while setting expectations for what a successful partnership and outcome looks like. This minimizes miscommunication and opportunity for expectations falling through. 2nd - Waiting till the last minute to find suppliers can lead hasty decision making which may get you out of a jam in the moment but lead to larger problems down the road. For this reason it’s vital you are proactive in establishing relationships with vendors and suppliers so they’re there when you need them. Establish Minimum Expectations for Vetting Suppliers Establishing minimum expectations means that you will vet all potential suppliers with the same list of needs and expectations. This will help to create an even playing field when vetting suppliers and their capabilities. Similar to #1, when you know what you want and have created a way to gather information which allows you to do equal comparisons your chance of making the right decision increases dramatically. Create an SOP or checklist to hold yourself accountable to collect the right information. Be Strategic Once you know what you need from a supplier it is important to think about other associated or cross functional activities which need to be done that could be accomplished by said supplier(s). The ideal situation is you find a supplier that can do more than just one component of your needs, therefore providing more value in the long run. This also saves you time because you have less suppliers and vendors to managed increasing your efficiency and effectiveness. Supplier Identification Referrals, referrals, referrals. Once you know what you need the best approach to finding the right supplier is by reaching out to others in your industry, or industry associations, to learn who they use, and just as important who they don’t use. Take the time to read reviews, gather intel from people you trust before you start calling potential suppliers. While sites like Thomas.net and Google can provide this information, it is likely you will quickly find yourself overwhelmed with information. In the end the most useful data is those which are unbiased or comes from experience -this is best collected from a trusted resource. Outreach and Selection When speaking for the first time with a potential new supplier try to connect with the people you will actually be working with, not just the company’s sales person. This is important because once the relationship is established the majority of your time won’t be spent with their sales people rather those delivering the service or product. What is their communication like? Do they respond quickly and address mistakes immediately? What is their customer retention rate? Find out how long their employees have been with the company too. If the company suffers from consistent turnover that should be a big red flag as you will likely have to be much more involved with this supplier helping coach and direct new employees to ensure the work is done properly. Also, where are you in the pecking order of the level of importance to the supplier? Don’t be fooled not all clients are treated equal, even if they tell you otherwise. When you know where you stand it is easier to build a relationship based on realistic expectations. In the end, supplier selection should come down to three things, in ranked order: 1. Performance 2. Relationship 3. Price Key Takeaway At the end of the day it doesn’t matter how affordable or cost effective a supplier is, or how nice they are as people. If they can’t perform, and do so consistently, the other two don’t matter. I’ve also found that paying a bit more for the right service and relationship often times is worth the investment it in the long run. #whitepaper #supplychain #supplier #vendor #selectionprocess #outsource #square1engineering #medtech #medicaldevice About the AuthorTravis Smith is the founder and managing director of Square-1 Engineering, a medical device consulting firm, providing end to end engineering and compliance services. He successfully served the life sciences marketplace in SoCal for over 15 years and has been recognized as a ‘40 Under 40’ honoree by the Greater Irvine Chamber of Commerce as a top leader in Orange County, CA. Categories
All
Archives
April 2024
|
Visit Square-1's
|
|








 RSS Feed
RSS Feed


